Telemedicine has really changed healthcare, especially for folks in rural areas where getting to a doctor can be a real hassle. Basically, it connects patients with healthcare providers remotely using technology – think video calls, online portals, and even remote monitoring devices. This means people in isolated communities can access specialists, get routine check-ups, and manage chronic conditions without long drives or time off work, which is a huge deal for their health and well-being.
One of the biggest struggles in rural healthcare is, well, distance. Living far from major towns or cities means fewer doctors, fewer specialists, and sometimes no hospital at all. Telemedicine steps in to bridge that gap, making quality healthcare more accessible than ever before.
Access to Specialized Care
Getting to see a specialist, like a cardiologist or a mental health professional, can be a real challenge in rural areas. Often, the nearest one is hours away.
Breaking Geographic Barriers
Imagine someone with a complex heart condition needing regular consultations. Instead of a day-long trip, they can now have a video visit with their cardiologist from their living room. This saves them travel time, fuel costs, and often, the need to take a day off work. It also means they can receive timely follow-up care that might have been postponed or skipped entirely due to logistics.
Expanding the Provider Pool
Telemedicine doesn’t just bring specialists closer; it effectively expands the pool of available providers. A rural clinic might not be able to recruit an endocrinologist, but with telemedicine, they can connect their patients to one in a larger city. This is transformative for conditions requiring highly specialized knowledge or interventions.
Addressing Primary Care Shortages
It’s not just specialists; even primary care doctors are in short supply in many rural regions. Telemedicine can help fill this void, ensuring people get basic medical attention.
Virtual Consultations for Common Ailments
For minor illnesses like a cold, flu, or simple skin rash, a virtual visit can be just as effective as an in-person one. A doctor can assess symptoms, provide advice, and even prescribe medication remotely. This frees up limited in-person appointments for more serious issues and reduces unnecessary visits to already strained emergency rooms.
Mental Health Support
Mental health services are notoriously scarce in rural areas. Telepsychiatry and teletherapy have become vital tools, offering confidential and convenient access to mental health professionals. This is particularly important given the stigma often associated with mental health in smaller communities, as a virtual session can feel more private.
In exploring the transformative effects of telemedicine on rural healthcare, it is essential to consider the technological tools that facilitate remote consultations and patient management. A related article that discusses the importance of having the right equipment for effective remote work can be found at Discover the Best Laptop for Remote Work Today. This resource highlights the significance of selecting appropriate technology, which is crucial for healthcare providers in rural areas to deliver quality care through telemedicine platforms.
Key Takeaways
- Clear communication is essential for effective teamwork
- Active listening is crucial for understanding team members’ perspectives
- Setting clear goals and expectations helps to keep the team focused
- Regular feedback and open communication can help address any issues early on
- Celebrating achievements and milestones can boost team morale and motivation
The Economic Benefits: More Than Just Health
Telemedicine isn’t just good for health; it also brings significant economic advantages to both patients and healthcare systems in rural areas.
Cost Savings for Patients
When you live remotely, healthcare costs aren’t just about the medical bill. There are often hidden expenses that add up quickly.
Reducing Travel Expenses
Consider the cost of gas for a two-hour drive, wear and tear on a vehicle, and potentially even overnight accommodation if follow-up appointments are needed. Telemedicine eliminates these costs. For many low-income families in rural areas, these savings are substantial and can make the difference between getting care and foregoing it.
Less Time Off Work
Taking a day off work for a doctor’s appointment means lost wages. For hourly workers, this can be a significant financial hit. Telemedicine appointments are often shorter and can be scheduled more flexibly, allowing individuals to maintain their work schedules with minimal disruption.
Efficiency for Healthcare Providers
Rural clinics often operate on tight budgets and with limited staff. Telemedicine can help them make the most of their resources.
Better Appointment Management
Virtual appointments can sometimes be quicker than in-person ones, especially for routine check-ups or follow-up questions. This can allow providers to see more patients in a day, improving overall efficiency and reducing wait times. It also reduces no-shows, as patients are less likely to miss an appointment that doesn’t require travel.
Optimized Resource Allocation
By triaging patients virtually, clinics can reserve in-person appointments for those who truly need hands-on examination or procedures. This means medical equipment and examination rooms are used more effectively, and staff time is better spent, leading to a more streamlined operation.
Overcoming Hurdles: The Challenges of Implementation

While the benefits are clear, rolling out telemedicine in rural areas isn’t without its obstacles. These challenges need thoughtful solutions for successful integration.
The Digital Divide
Not everyone in rural areas has equal access to the internet or the necessary technology. This is a critical hurdle.
Internet Connectivity Issues
Many rural areas still lack reliable, high-speed broadband internet.
A video consultation requires a stable connection, and without it, telemedicine is simply not possible. This “digital divide” disproportionately affects older populations and lower-income families who may not be able to afford internet access even if available. Government initiatives and private partnerships are crucial here to expand broadband infrastructure.
Lack of Devices or Digital Literacy
Even with internet, some individuals may not own a smartphone, tablet, or computer, or might not be comfortable using them for medical appointments.
This calls for community-based solutions, such as providing access to devices at local libraries or community centers, and offering digital literacy training programs.
Regulatory and Reimbursement Complexities
The healthcare system is heavily regulated, and telemedicine has had to navigate a patchwork of rules and payment structures.
Varying State Laws
Regulations around telemedicine, including what services can be provided and across state lines, vary significantly from state to state. This can create confusion for providers and limit the reach of telemedicine services, especially for patients near state borders. Efforts for more uniform national guidelines would be beneficial.
Insurance Coverage Issues
While coverage for telemedicine has expanded significantly, especially during the pandemic, it’s not always consistent.
Some services might not be covered, or reimbursement rates might be lower than for in-person visits. This can create financial disincentives for providers to adopt telemedicine widely. Advocacy for equitable reimbursement is ongoing.
Enhancing Quality of Care: Beyond Just Access

Telemedicine doesn’t just make healthcare more accessible; in many instances, it can actually improve the quality and continuity of care for rural patients.
Better Management of Chronic Conditions
Managing ongoing health issues like diabetes, heart disease, or asthma requires consistent monitoring and frequent check-ins. Telemedicine is perfectly suited for this.
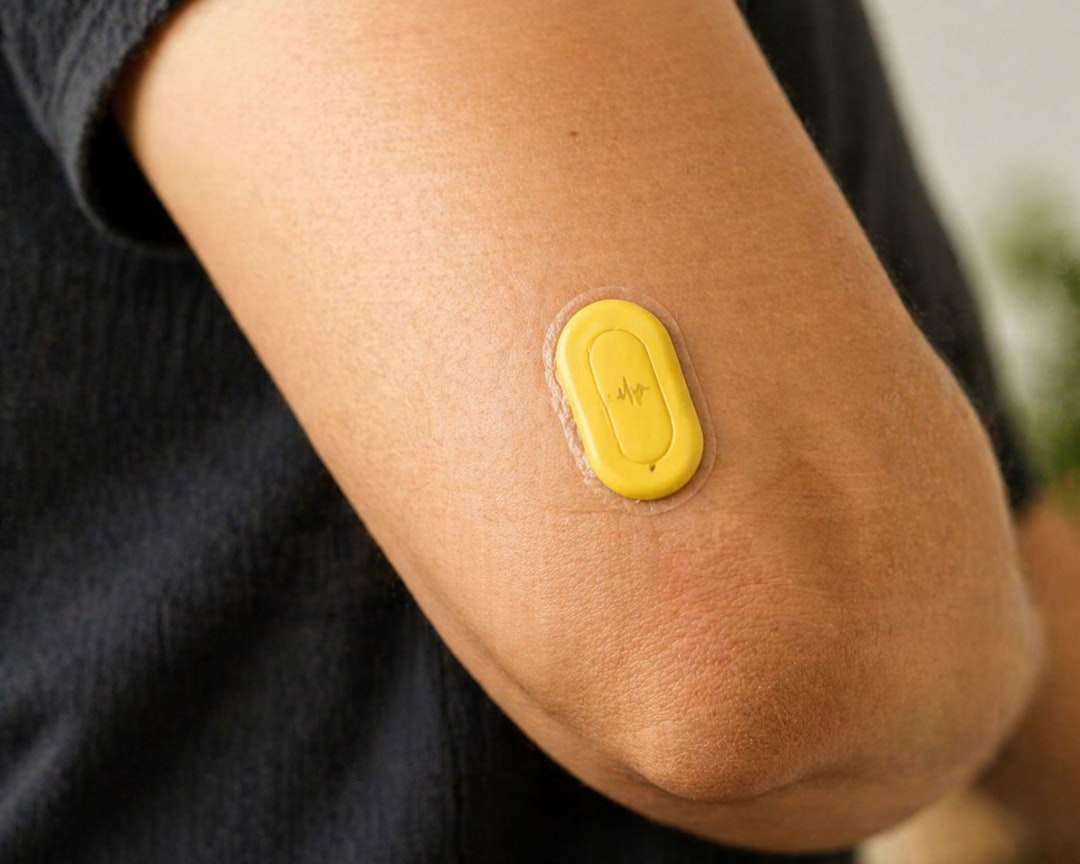
Remote Monitoring Devices
Wearable devices and at-home medical equipment can collect vital signs like blood pressure, blood sugar, and oxygen levels, transmitting data directly to providers. This allows doctors to keep a close eye on their patients’ conditions and intervene quickly if something changes, often before it becomes an emergency. For example, a diabetic patient can share their blood glucose readings daily, allowing their doctor to adjust medication proactively.
Regular Follow-Ups and Education
Instead of waiting months for an in-person appointment, patients can have more frequent, shorter virtual check-ins. This fosters better adherence to treatment plans and provides opportunities for ongoing patient education, empowering individuals to take a more active role in managing their own health. These routine interactions can also build stronger patient-provider relationships, even remotely.
Reducing Hospital Readmissions
For patients discharged from the hospital, the period immediately following is critical for preventing complications and readmission. Telemedicine can play a key role in this vulnerable time.
Post-Discharge Monitoring and Support
Virtual check-ups and remote monitoring can help identify potential issues early, ensuring patients are recovering well and following discharge instructions. A quick video call with a nurse can answer questions about medication or wound care, preventing a return trip to the emergency room.
Transition of Care Coordination
Telemedicine facilitates better communication between hospital staff, primary care providers, and patients as they transition home. This coordinated approach ensures continuity of care and reduces the likelihood that important information or follow-up needs fall through the cracks. It creates a safety net for patients who might otherwise feel isolated after leaving the hospital.
The integration of telemedicine into rural healthcare has significantly transformed patient access and treatment options, addressing long-standing challenges faced by these communities. For a deeper understanding of how technology influences various fields, you might find it interesting to explore the article on selecting the best laptop for architects, which highlights the importance of having the right tools for effective design and planning. This connection illustrates how advancements in technology can enhance not only healthcare but also other professional domains. You can read more about it here.
The Future Landscape: What’s Next for Rural Telemedicine?
| Metrics | Data |
|---|---|
| Increased Access to Healthcare | 70% of rural patients have improved access to healthcare services through telemedicine. |
| Cost Savings | Telemedicine has saved rural patients an average of 2,500 per year in travel and related costs. |
| Improved Health Outcomes | Telemedicine has led to a 25% reduction in hospital readmission rates for rural patients. |
| Provider Shortage Mitigation | Telemedicine has helped to address the shortage of healthcare providers in rural areas by connecting patients with specialists remotely. |
Telemedicine in rural areas is still evolving. We can expect to see further advancements and broader integration as technology progresses and policies adapt.
Technological Innovations
The pace of technological development means we’ll likely see even more sophisticated tools emerge.
AI and Machine Learning in Diagnostics
Artificial intelligence could assist in analyzing medical images or patient data, helping rural providers with diagnoses, especially in specialties where local expertise is limited.
Imagine an AI tool assisting a general practitioner in a rural clinic to interpret a complex echocardiogram.
While not replacing the expert, it could provide valuable support.
Advanced Remote Sensing
Beyond current wearables, future remote sensing technologies could offer even more comprehensive physiological monitoring, potentially detecting subtle changes in health status before symptoms even appear. This proactive approach could be a game-changer for preventative care in remote settings.
Policy and Funding Support
Continued government and organizational backing will be crucial for sustained growth.
Sustained Reimbursement Parity
Advocacy for permanent reimbursement parity – meaning telemedicine visits are paid at the same rate as in-person visits – is essential. This stability encourages providers to invest in telemedicine infrastructure and training, making it a sustainable part of their practice model. Without it, the expansion of telemedicine, particularly in underserved areas, could stall.
Investment in Rural Broadband Infrastructure
The “digital divide” remains a significant barrier. Continued and increased funding for rural broadband expansion will be fundamental. This isn’t just about healthcare; it’s about economic development and access to education as well. Investing in robust internet infrastructure is an investment in the future of rural communities.
In essence, telemedicine isn’t just a temporary fix; it’s a fundamental shift in how healthcare can be delivered, offering a lifeline to rural communities. While challenges remain, the clear benefits in terms of access, cost-effectiveness, and quality of care make it an indispensable tool for ensuring everyone, no matter where they live, has the opportunity for good health.
FAQs
What is telemedicine?
Telemedicine is the use of technology to provide healthcare services remotely. This can include video consultations, remote monitoring of patients, and the exchange of medical information through digital communication.
How does telemedicine impact rural healthcare?
Telemedicine has a significant impact on rural healthcare by providing access to medical specialists and services that may not be readily available in rural areas. It helps bridge the gap between rural patients and healthcare providers, improving access to care and reducing the need for travel.
What are the benefits of telemedicine for rural communities?
The benefits of telemedicine for rural communities include improved access to healthcare, reduced travel time and costs for patients, increased efficiency in delivering care, and the ability to receive specialized medical services without having to leave the community.
What are the challenges of implementing telemedicine in rural areas?
Challenges of implementing telemedicine in rural areas include limited access to high-speed internet, lack of technological infrastructure, concerns about data security and privacy, and the need for training and education for healthcare providers and patients.
How does telemedicine impact the quality of care in rural areas?
Telemedicine can improve the quality of care in rural areas by enabling timely access to medical expertise, facilitating better coordination of care between healthcare providers, and reducing the barriers to accessing necessary medical services.